21. Screening Mammography and Breast Cancer Detection
 Chapter
21. Rethink Pink October Breast Cancer
Mammogram
Chapter
21. Rethink Pink October Breast Cancer
Mammogram
Rethink Pink October Breast Cancer Month - A Closer Look at Screening Mammography
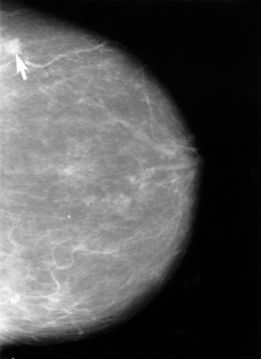
Left Image: Screening Mammogram showing small cancer (upper left arrow), courtesy of the National Institute of Health and wikimedia commons.
A bombshell article appeared in October 2009 JAMA (the Journal of the American Medical Association) questioning mammography breast cancer screening. (1) Dr. Laura Esserman reviewed 20 years of data and concludes that screening the population for breast cancer has significant drawbacks. The expected survival benefits have not materialized. She says that it is true that early stage breast cancer has decreased due to mammography, however, the data shows no decrease in the advanced, “killer” cancers. Overall mortality rates from breast cancer have declined slightly; however, Dr Esserman attributes this to better treatment rather than to screening mammography.
Detected Cases Go Up With Screening Mammography
The combined 20 years of breast cancer data shows essentially no change in the annual cases of breast cancer cases detected, until 1983 when screening mammography was introduced, with an immediate spike and dramatic increase in the number of breast cancer cases detected annually, thanks to this new diagnostic tool, the mammogram.
More Cased Detected, But Only a Modest Decline in Cancer Mortality
Although screening mammography detects dramatically more cases of breast cancer, this increased detection has not translated into decreased mortality in the population. Yes, mortality numbers have decreased slightly. The annual mortality rate for breast cancer from 1930 to 2006 was stable at about 30 cases per 100,000 women, and declined over the last few years to about 25 cases per 100,000. However, this is not due to screening mammography. Dr. Esserman suggests this rather modest decline in mortality is due to improvement in treatment, not increased detection. (1)
Annual Breast Cancer Mortality - Where's the Benefit?
While the incidence of early stage breast cancer has decreased by 2.8 per cent per year since 2001, incidence rates of advanced (distant-stage) disease have remained remarkably stable over this same time period. In 2009, 192,370 women were diagnosed with breast cancer and 40,170 women died of breast cancer. Mammography has increased the detection of very early stage cancer, called DCIS (ductal carcinoma in situ), with 60,000 cases of DCIS detected annually, however, the number of advanced breast cancer cases, the serious fatal type, has not changed by the introduction of mammography screening. This lack of benefit is disappointing.
Dr. Esserman's 2009 Observations Were Made in 2002 by Barnett Kramer
Dr. Barnett Kramer, director of the Office of Disease Prevention at the National Institutes of Health, was interviewed in a 2002 article in the New York Times, in which he said:
"The number of women with breast cancers with the worst prognosis, those that spread to other organs, had been fairly constant in the years before mammography was introduced, and that trend did not change after the introduction of mammography...If screening worked perfectly, every cancer found early would correspond to one fewer cancer found later. That did not happen. Mammography, instead has resulted in a huge new population of women with early stage cancer but without a corresponding decline in the numbers of women with advanced cancer." (31)
|
Important Point: Mammography Has Failed to Live Up To Expectations |
|
Screening Mammography has not lived up to expectations. Although more cases of early breast cancers are found, this has not reduced the number of late stage or killer cancers. |
Weighing the Pluses and Minuses of Screening Mammography
Dr Gilbert Welch in his BMJ editorial says the following about mammography screening for breast cancer: (7)(8)(9)
1
in 1,000 women annually screened for 10 years will avoid dying from breast
cancer.
2 to 10 women will be over-diagnosed and treated needlessly.
10 to 15 women will be told they have breast cancer earlier than they would
otherwise have been told, but this will not affect their prognosis.
100 to 500 women will have at least one "false alarm" (about half of
these women will undergo a biopsy)
Mammography - Finding the Reservoir of DCIS
Mammography screening finds the small indolent cancers called DCIS, ductal carcinoma in situ, that represent a reservoir of silent disease in up to 18% of the population, demonstrated by autopsy studies.(18) This leads to over diagnosis and overtreatment. For the invasive cancers which we know are present in one to two per cent of the population, (demonstrated by autopsy series), screening detection is of little help, with little change in the number of advanced cancer cases, and about 40,000 deaths every year. Dr. Gilbert Welch sums it up with the following sage advice: "doctors who recommend less-aggressive mammography (less frequently, waiting until you are age 50, or stopping it when you are older) or are less quick to biopsy may not be bad doctors but good ones."
|
Important Point: |
|
The reason why mammography has had little impact on breast cancer mortality is that mammography is an X-Ray imaging technique that finds small calcifications indicating DCIS, an indolent, non-aggressive lesion with a good prognosis. (42-50). The data suggests that finding and aggressively treating DCIS does not reduce mortality rates from advanced breast cancer. |
Just Stop Calling It Cancer
One glaring problem with screening mammography is the detection of DCIS at a rate of 60,000 cases per year.(17) DCIS is ductal carcinoma in situ, a pathology diagnosis which carries a very good prognosis, a 98 per cent - five year survival. In spite of the rather benign natural history of DCIS, mainstream medicine treats these lesions aggressively with surgery and radiation. Recently, the NIH has called for a change in terminology, asking pathologists to stop calling it "cancer". Here is the NIH consensus statement:
"Because of the noninvasive nature of DCIS, coupled with its favorable prognosis, strong consideration should be given to elimination of the use of the anxiety-producing term “carcinoma” from the description of DCIS.”(2)
Dr Fletcher in the New England Journal Sums IT UP
Dr Suzanne Fletcher summed up the issues with screening mammography detection of DCIS nicely in her 2003 article published in the New England Journal with this quote: (38)
“…the risk of death from breast cancer within 10 years after the diagnosis of DCIS (ductal carcinoma in situ) was 1.9 percent. Such an excellent prognosis could be attributable to the detection of lesions before they become invasive cancers, which could save lives. However, if ductal carcinoma in situ were the usual precursor to early invasive cancer, the incidence of early-stage invasive breast cancer should decrease as the incidence of in situ cancer increases, but the opposite is happening. Also, autopsy studies in women who died from causes unrelated to breast cancer have shown a substantial “reservoir” of ductal carcinoma in situ in such women. (Welch)(18) Therefore, detection of ductal carcinoma in situ may be an example of overdiagnosis — finding early neoplasms, many of which will never become invasive breast cancer. Unfortunately, ductal carcinoma in situ can progress to invasive cancer. The eight-year rate of recurrence in one study of treatment with only surgical excision was 27 percent, and half the recurrences were invasive cancers. It is not clear who is at risk for recurrence and whether survival results would be the same if surgery were undertaken only after early invasive cancer had been diagnosed. In sum, women who undergo screening mammography are more likely than other women to be given a diagnosis of ductal carcinoma in situ. Whether finding it (DCIS) saves lives or merely increases the number of women who receive a diagnosis of breast cancer is not yet clear. “endquote Dr Fletcher NEJM.(38)
We Just Don’t Know the Natural Course of Untreated DCIS
A large part of the problem is that we simply do not have a good understanding of the natural course of DCIS. Although we know that some cases of DCIS will progress to invasive cancer, many will not. We have no reliable tools to distinguish the “stable/benign” DCIS cases from the “aggressive” DCIS cases destined to become invasive. Dr. Erbas says, “The available evidence suggests not all DCIS will progress to invasive cancer in the medium term but precise estimates of progression are not possible given the limitations of the data. “(39) Hopefully, in the near future, new diagnostic tools will be developed to tell us which DCIS cancers need more aggressive treatment and which ones need less aggressive treatment.
Invasive Breast Cancer 15 to 30 years after diagnosis of DCIS !!
Another striking finding is that when following DCIS cases over 30 years, invasive cancers are found fifteen to twenty five years after the initial biopsy. (40-41) . This is remarkable. In my opinion, this reflects an underlying nutritional deficiency, biochemical or genetic abnormality which places the patient at increased risk for breast cancer during their lifetime.
DCIS: An Iodine Deficiency Disease?
Breast tissue takes up Iodine by virtue of an active transport called the NIS, Sodium Iodide Symporter. (54-55) In addition, iodine deficiency is a known risk factor for breast cancer, and iodine has been suggested as an adjuvant treatment for breast cancer.(51-53) Are DCIS patients Iodine deficient, and that is why these individuals have a propensity for breast cancer ? Unfortunately, most breast cancer studies ignore Iodine, and do not measure urinary Iodine levels, so we don’t know the answer. In a few anecdotal cases with a history of treated breast cancer, we have found profoundly low iodine levels. Perhaps new studies sponsored by NIH funding can answer this question. However, in the mean time, it is reasonable to test Iodine levels and provide Iodine supplements to patients at risk for breast cancer or recurrence. Urinary spot iodine testing is widely available at all national labs.
|
Important Point: |
|
Iodine supplementation is our best tool for breast cancer prevention. |
How to Prevent Breast Cancer – Our Program
1) Iodine Supplementation ( Iodoral tablets)
2) Natural Progesterone, topical cream
3) Avoid carcinogenic chemicals, xenoestrogens, pesticides, etc.
4) Vitamin D Supplementation. (Vitamin D3 capsules)
For references and links, see my web site: www.bioidenticalhormones101.com
References for Chapter 21. Rethink Pink October Breast Cancer Mammogram
(1) http://jama.highwire.org/cgi/content/abstract/302/15/1685
Rethinking
Screening for Breast Cancer and Prostate Cancer. Laura Esserman, MD, MBA; Yiwey
Shieh, AB; Ian Thompson, MD JAMA. 2009;302(15):1685-1692.
(2) http://consensus.nih.gov/2009/dcisstatement.htm NIH Consensus statement on DCIS
2009
(3) http://www.medpagetoday.com/HematologyOncology/BreastCancer/16538 Analysis Questions Breast and
Prostate Cancer Screening By Peggy Peck, Executive Editor, MedPage
Today October 21, 2009
(4) http://movingtotheusa.blogspot.com/2009/10/rethinking-strategies-for-breast-and.html
Thursday, 22 October 2009. Rethinking strategies for breast and prostate cancer
screening.
(5) http://www.vaoutcomes.org/welch.php H. Gilbert Welch, MD, MPH
Professor of Medicine and Community and Family Medicine, Dartmouth Medical
School; Co-Director of the White River Junction Outcomes Group
(6) http://www.vaoutcomes.org/papers/NYT_cancer_screening.pdf How Two Studies on Cancer Screening Led to Two Results - New York Times March 13, 2007
(7) http://8.12.42.31/2008/nov/03/opinion/oe-welch3 The excessive focus on mammography. Looking harder to find more may not be the best practice. By H. Gilbert Welch November 03, 2008
(8) http://www.nytimes.com/2008/10/07/health/views/07essa.html Campaign Myth: Prevention as Cure-All By H. GILBERT WELCH, M.D October 6, 2008
(9) http://www.bmj.com/cgi/content/full/339/jul09_1/b1425 9 July 2009, BMJ 2009;339:b1425 Editorials. Gilbert Welch MD. Overdiagnosis and mammography screening.
(10) http://www.huffingtonpost.com/helen-cordes/rethink-pink-now-saner-so_b_329496.html
Rethink Pink NOW! Saner Solutions to Breast Cancer, Part 2 Huffington Post,
Helen Cordes.
(11) http://archinte.ama-assn.org/cgi/content/abstract/168/21/2311
The Natural
History of Invasive Breast Cancers Detected by Screening Mammography by Per-Henrik
Zahl, MD, PhD; Jan Mæhlen, MD, PhD; H. Gilbert Welch, MD, MPH Arch Intern Med.
2008;168(21):2311-2316.
(12) http://www.nytimes.com/2008/11/25/health/25breast.html?pagewanted=1&_r=2
Study Suggests Some Cancers May Go Away By GINA KOLATA November 24, 2008.
New York Times.
(13) http://jeffreydach.com/2009/10/01/psa-testing-the-failed-medical-experiment-by-jeffrey-dach-md.aspx PSA
Screening for Cancer, the Failed Medical Experiment by Jeffrey Dach MD
(14) http://www.greenhealthspot.com/2009/10/rethinking-cancer-screening.html
Rethinking Cancer Screening Dr Wang
(15) http://www.dbtechno.com/health/2009/10/21/study-says-screening-for-breast-cancer-is-over-rated/
Study says screening for breast cancer is over rated, dbtechno blog.
(16) http://jeffreydach.com/2009/08/16/the-thyroid-nodule-epidemic-by-jeffrey-dach-md.aspx
The Thyroid Nodule Epidemic by Jeffrey Dach MD
(17) http://theoncologist.alphamedpress.org/cgi/content/full/12/11/1276 The Oncologist, Vol. 12, No. 11,
1276-1287, November 2007; Current Treatment and Clinical Trial Developments for
Ductal Carcinoma In Situ of the Breast. Judy C. Bougheya, Ricardo J.
Gonzalezb, Everett Bonnerc, Henry M. Kuererb
(18) http://www.annals.org/cgi/content/full/127/11/1023 Using Autopsy Series To Estimate
the Disease "Reservoir" for Ductal Carcinoma in Situ of the Breast:
How Much More Breast Cancer Can We Find? H. Gilbert Welch, MD, MPH,
and William C. Black, MD Annals of Internal Med, December 1 1997,| Volume 127,
Issue 11, Pages 1023-1028.
(19) http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2002422/?tool=pubmed Br J Cancer. 1987 December; 56(6): 814–819. Breast cancer and atypia among young and middle-aged women: a study of 110 medicolegal autopsies. M. Nielsen et al.
(20) http://www.cancer.org/downloads/STT/F861009_final%209-08-09.pdf
Breast Cancer Facts and Figures 2009,2010 American Cancer Society
(21) http://www.cancer.org/docroot/stt/stt_0.asp Breast cancer facts and figures
2009 ACS
(22) http://seer.cancer.gov/statfacts/html/breast.html SEER Cancer Statistics. It is
estimated that 192,370 women will be diagnosed with and 40,170 women will die
of cancer of the breast in 2009.
(23) http://seer.cancer.gov/csr/1975_2006/results_merged/sect_04_breast.pdf NCI’s SEER Cancer Statistics
Review, Incidence & Mortality Breast Cancer
(24) http://caonline.amcancersoc.org/cgi/content/full/59/4/225 CA Cancer J Clin 2009;
59:225-249 Cancer Statistics, 2009 Ahmedin Jemal, DVM, PhD1, Rebecca Siegel,
MPH2, Elizabeth Ward, PhD3, Yongping Hao, PhD4, Jiaquan Xu, MD5 and Michael J.
Thun, MD, MS6
(25) http://seer.cancer.gov/csr/1975_2006/results_single/sect_01_table.01.pdf NCI’s SEER Cancer Statistics
Review, Incidence & Mortality Breast Cancer
(26) http://www.alternet.org/healthwellness/143195/saving_women_from_breast_cancer%3A_are_mammograms_really_the_answer/
Saving Women From Breast Cancer: Are Mammograms Really the Answer? By
Naomi Freundlich, Health Beat. Posted October 21, 2009.
(27) http://www.timesonline.co.uk/tol/comment/letters/article5761650.ece?token=null&offset=0&page=1
February 19, 2009. Breast cancer screening peril. Negative consequences of the
breast screening programme.
(28) http://breastcanceradvocate.wordpress.com/
2009/10/01/the-truth-about-breast-cancer-is-not-pretty-and-its-not-pink/
The Truth About Breast Cancer is Not Pretty and it’s not Pink Posted October 1,
2009
(29) http://ww5.komen.org/contentsimpleleft.aspx?id=6442451356&itc=lefthpban:77 Comments on Mammography Leading to Over-Diagnosis and Over-Treatment (Dr. Eric Winer, October 2009)
(30) http://www.cbcrp.org/publications/papers/Mayer/page_08.php Changes in Breast Cancer
Mortality Rates,
(31) http://www.nytimes.com/2002/04/09/
science/confronting-cancer-breast-cancer-mammography-finds-more-tumors-then-debate.html
CONFRONTING CANCER; Breast Cancer: Mammography Finds More Tumors. Then the Debate
Begins. By Gina Kolata Published: Tuesday, April 9, 2002. New York Times.
(32) http://nosurrenderbreastcancer.blogspot.com/2009/10/acs-throws-women-under-bus.html
Wednesday, October 21, 2009. ACS Throws Women Under the Bus.
(33) http://www.ratical.org/radiation/CNR/XHP/MPDaXrayST.html Making Personal Decisions
about X-ray Screening Tests, Such as Mammography and CT of the Lung,
Colon, Heart, or the Entire Body. John W. Gofman, M.D., Ph.D
(34) http://www.noetic.org/research/sr/main.html Database of spontaneous
remission.
(35) The
Medical Aspects of Carcinoma of the Breast, with a Note on the Spontaneous
Disappearance of Secondary Growths OSLER W American Medicine: April 6 1901;
17-19; 63-66 Extracted Summary
(36) http://www.auntminnie.com/index.asp?sec=ser&sub=def&pag=dis&ItemID=87566 'Spontaneous regression' debate
erupts anew at ASCO symposium, by Kate Madden Yee AuntMinnie.com staff writer
October 12, 2009.
(37) http://www.ncbi.nlm.nih.gov/pmc/articles/PMC164507/ Proc Natl Acad Sci U S A. 2003 May 27; 100(11): 6682–6687. The National Academy of Sciences. Immunology Spontaneous regression of advanced cancer: Identification of a unique genetically determined, age-dependent trait in mice. Zheng Cui et al.
(38) http://www.cwru.edu/CWRU/Med/medicine/newsite/internal/screenbreastcancer.pdf
N Engl J Med 2003;348:1672-80. Mammographic Screening for Breast Cancer Suzanne
W. Fletcher, M.D., and Joann G. Elmore, M.D., M.P.H. With treatment, the prognosis is excellent.
(39) http://www.springerlink.com/content/pm20211j67150mw4/ Breast Cancer Research and Treatment Volume 97, Number 2, 135-144. The natural history of ductal carcinoma in situ of the breast: a review by Bircan Erbas et al.
(40) http://onlinelibrary.wiley.com/doi/10.1002/1097-0142(19951001)76:7%3C1197::AID-CNCR2820760715%3E3.0.CO;2-0/pdf Cancer Volume 76, Issue 7, pages 1197–1200, 1 October 1995. Continued local recurrence of carcinoma 15–25 years after a diagnosis of low grade ductal carcinoma in situ of the breast treated only by biopsy. David L. Page M.D et al.
(41) http://www.ncbi.nlm.nih.gov/pubmed/6275978 Cancer. 1982 Feb 15;49(4):751-8. Intraductal carcinoma of the breast: follow-up after biopsy only. Page DL, Dupont WD, Rogers LW, Landenberger M.
(42) http://archinte.ama-assn.org/cgi/content/full/160/7/953 Arch Intern Med. 2000 Apr 10;160(7):953-8. Mortality among women with ductal carcinoma in situ of the breast in the population-based surveillance, epidemiology and end results program. Ernster VL, Barclay J, Kerlikowske K, Wilkie H, Ballard-Barbash R.
(43) http://www.ncbi.nlm.nih.gov/pubmed/11350725 Endocr Relat Cancer. 2001 Mar;8(1):33-45. The management of ductal carcinoma in situ of the breast. Skinner KA, Silverstein MJ.
(44) http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1557717/?tool=pubmed Breast Cancer Res. 2006; 8(2): 204. Overdiagnosis and overtreatment of breast cancer: Progression of ductal carcinoma in situ: the pathological perspective. J Louise Jones Tumour Biology Laboratory,
(45) http://www.ncbi.nlm.nih.gov/pubmed/10772968 Cancer Treat Rev. 2000 Apr;26(2):103-25. Ductal carcinoma in situ (DCIS) of the breast: evolving perspectives. Sakorafas GH, Tsiotou AG.
(46) http://www.ncbi.nlm.nih.gov/pubmed/14626378 Int J Fertil Womens Med. 2003
Sep-Oct;48(5):217-25. Treatment of ductal carcinoma in situ of the breast:
review of recent advances and future prospects. Mokbel K.
(47) http://www.ncbi.nlm.nih.gov/pubmed/15884091 Cancer. 2005 Jun 15;103(12):2481-4.
The natural history of low-grade ductal carcinoma in situ of the breast in
women treated by biopsy only revealed over 30 years of long-term follow-up. Sanders
ME, Schuyler PA, Dupont WD, Page DL.
(48) http://www.ncbi.nlm.nih.gov/pubmed/17687650
Breast Cancer Res Treat. 2008 Jun;109(3):405-16. 259 Patients with DCIS of the breast applying
USC/Van Nuys prognostic index: a retrospective review with long term follow up.
Di Saverio S, Catena F, Santini D, Ansaloni L, Fogacci T, Mignani S, Leone A,
Gazzotti F, Gagliardi S, De Cataldis A, Taffurelli M.
(49) http://jnci.oxfordjournals.org/content/96/12/906.full Ductal Carcinoma In Situ,
Complexities and Challenges JNCI J Natl
Cancer Inst (2004) 96 (12): 906-920.
(50) http://annonc.oxfordjournals.org/content/13/8/1236.full Management of women with ductal carcinoma in situ of the breast: a population-based study . H. M. Verkooijen et al. Ann Oncol (2002) 13 (8): 1236-1245.
(51) http://iodine4health.com/research/cann_2000_iodine_selenium_breast_cancer.pdf
Cancer Causes and Control 11: 121±127, 2000. 121. Hypothesis: Iodine, selenium and the development of breast cancer. Stephen A. Cann et al.
(52) http://www.ncbi.nlm.nih.gov/pubmed/16025225 J Mammary Gland Biol Neoplasia. 2005 Apr;10(2):189-96. Is iodine a gatekeeper of the integrity of the mammary gland? Aceves C, Anguiano B, Delgado G.
(53) http://www.ncbi.nlm.nih.gov/pubmed/17956159 Thyroid. 2007 Sep;17(9):851-9. Uptake and gene expression with antitumoral doses of iodine in thyroid and mammary gland: evidence that chronic administration has no harmful effects. Anguiano B, García-Solís P, Delgado G, Aceves Velasco C.
(54) http://www.ncbi.nlm.nih.gov/pubmed/9735978 Clin Nucl Med. 1998 Sep;23(9):585-7. I-131 uptake in the breast for thyroid cancer surveillance with biopsy-proven benign tissue. Allen T, Wiest P, Vela S, Hartshorne M, Crooks LA.
(55) http://www.ncbi.nlm.nih.gov/pubmed/20201784 Curr Cancer Drug Targets. 2010 Mar;10(2):242-67. The biology of the sodium iodide symporter and its potential for targeted gene delivery. Hingorani M et al.

 Chapter
21. Rethink Pink October Breast Cancer
Mammogram
Chapter
21. Rethink Pink October Breast Cancer
Mammogram