 PCOS Polycystic Ovary Syndrome PCOS Polycystic Ovary Syndrome
Part One
Anovulatory Androgen Excess
by Jeffrey Dach MD
Seventeen
year old Alice has PCOS (Polycystic Ovary Syndrome). Alice came
with her Mom into the office and told me her story. Alice has been
overweight, borderline diabetic, and has facial hair and acne caused by
elevated testosterone. At age 12, Alice started normal menstrual
cycles, but her cycles began fluctuating and periods stopped at age 15.
Her gyne doctor diagnosed PCOS (Polycystic Ovary Syndrome), and put her
on birth control pills to regulate her cycles. The birth control pills
caused adverse side effects of weight gain weight and elevated blood
pressure (hypertension), so she stopped them.
Progesterone is the Most Logical Form of Treatment and Actually Works
Two months ago, Alice was switched over from the birth control pills to
natural progesterone, taking a 100 mg capsule twice a day for 14 days
on, 14 days off. The progesterone was successful, restoring a normal
menstrual period, and a return to regular cycles.
BCP’s (birth control pills) are usually prescribed by the ob-gyne doctor
to regulate cycles in the PCOS patient. This standard treatment is not
the best one. There is a better more logical alternative that actually
works called natural progesterone. Both John R Lee MD, and JeriLynn
Prior MD advocate the use of natural progesterone as a far better
alternative to birth control pills. After all, birth control
pills (BCP's) are a chemical form of castration, and work by inhibiting
ovulation.
This article will explain the cause of PCOS, and will describe the signs
and symptoms of PCOS, including the clinical features of PCOS, and give
you a simple questionnaire to determine if you have PCOS. This
article will also explain why natural progesterone is the best
treatment, and a much better choice compared to birth control pills.
PCOS was Rare When First Described in 1935, Now Quite Common.
When
PCOS (polycystic ovary syndrome) was first described in 1935 by Stein
and Leventhal, it was fairly rare.(55) Nowadays, it is quite common,
involving 6 to 10 per cent of the female population, affecting 3.5 to 5
million women. (24) Why the increased incidence? Some believe that endocrine disruptor chemicals in the environment are to blame.(60A)
 Clinical Signs and Symptoms Of PCOS Clinical Signs and Symptoms Of PCOS
Oligomenorrhea or amenorrhea (no periods), Anovulation (no ovulation)
Weight gain, obesity, Hirsutism (excessive hair growth, male pattern)
Insulin resistance (pre-diabetes), Acne, Male-pattern baldness, Multiple
small ovarian cysts on sonogram, Acanthosis Nigrans (darkening of the
skin at the nape of the neck and under arms)-indicator of
hyperinsulinemia
Above Left Image: Obese Young Lady with PCOS, anovulatory infertility, acne and facial hair.
A Brief Moment for Definitions:
Definition of ovulation: This
is the when an egg pops out of the follicle in the ovary, and starts on
the long trip down the fallopian tube to the uterine cavity where it
can be fertilized to form a new baby. Ovulation causes high progesterone
production by corpus luteum in the ovary. Menstrual Cycles are regular.
Definition of Anovulation: The egg doesn't’t pop out and there is no progesterone production. The cycles are irregular or absent.
Above Left Image: Typical hirsutism, with hair growth under the chin.
 How Do You Know If You Have PCOS? How Do You Know If You Have PCOS?
This is the PCOS Questionnaire.(63)(64) and these are the Links to questionnaire articles:
1) PCOS Questionnaire
2) PCOS questionnaire
If you answer Yes, to 2 out of 3 of the following questions, this indicates high likelihood (80%) of PCOS.
Above Left Image: The bearded fat lady at the circus. She had PCOS.
Length of Menstrual Cycle, Variable Length
1) Between the ages of 16 and 40, was length of your menstrual cycle (on average) greater than 35 days and/or totally variable ?
Hair Growth (Male Pattern)
2) During your menstruating years (not including during
pregnancy), did you have dark, coarse hair on your three or more of
these sites? Upper lip? chin? breasts? chest between the breasts? back?
belly? upper arms? upper thighs?
Obesity
3) Were you ever obese or overweight between the ages of 16 and 40?
 What Causes PCOS ? What Causes PCOS ?
The world’s greatest authority, Leon Speroff MD, says: “A question which
has puzzled gynecologists and endocrinologists for many years is what
causes polycystic ovaries. There is an answer which is appealing in its
logic and clinical applicability. The characteristic polycystic ovary
emerges when a state of anovulation persists for any length of time”
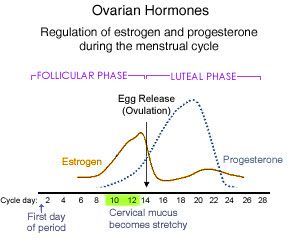
Left Chart: Hormone Levels during the Menstrual Cycle with normal
ovulation. The turquoise dotted line is progesterone which rises days
14-22. The progesterone is absent in PCOS, because there is no
ovulation, and progesterone line stays flat on the chart, instead of
rising
(1) Clinical Gynecologic Endocrinology and Infertility by Leon Speroff MD p.493
According to Dr. Speroff, PCOS is the end result of not ovulating, (no
progesterone production) for a long time (a few years), resulting in a
vicious cycle which self perpetuates anovulation, causing increased
testosterone production by the ovary. Insulin resistant diabetes and
obesity aggravate the problem. As you might expect, PCOS is a major
cause of infertility.
Update 2014: The Cause of PCOS
PCOS is explained as Hormone Receptor Defect Caused by Exposure to Hormone Disrupting Chemicals such as BPA. See this article: PCOS BPA Part 3 for more on this.
Non Classical CAH
About 10% of patients thought to have PCOS actually have an underlying
genetic enzyme defect in adrenal steroid synthesis called Non-Classical
CAH. This can be diagnosed with a Cortrosyn stimulation test, and a
21-OH genetic test called CAHDtex from Esoterix. If present, treatment
is successful with low dose adrenal steroid tablets (cortef,
dexamethasone, prednisone) which restores fertility and reverses the
acne. (see below discussion on non-classical CAH).
 Oral Contraceptives Oral Contraceptives
for PCOS (BCP's)
Birth control pills are a chemical form of castration, which prevent
ovulation. Lack of ovulation is the primary defect in PCOS, so birth
control pills merely perpetuate the primary defect. Birth control pills
can restore regular bleeding periods, however, this is artificial, and
aggravate the underlying PCOS problem rather than solve it. In addition,
birth control pills are known to worsen insulin resistance and
diabetes. (2)
"PCOS may affect between 3.5 and 5.0 million young women in the United
States, it arguably may be the most important general health issue
affecting young women. BCP's (OCPs) are the traditional therapy for the
chronic treatment of PCOS…… limited evidence raises the issue that BCP's
(OCPs) may aggravate insulin resistance and exert other untoward
metabolic actions that possibly enhance the long-term risk for diabetes
and heart disease."
 JeriLynn Prior MD Says: “The
fundamental problem with PCOS is not making progesterone for two weeks
every cycle. This lack of progesterone leads to an imbalance in the
ovary, causes the stimulation of higher male hormones and leads to the
irregular periods and trouble getting pregnant. Progesterone is usually
missing—replacing it therefore makes sense. “ JeriLynn Prior MD Says: “The
fundamental problem with PCOS is not making progesterone for two weeks
every cycle. This lack of progesterone leads to an imbalance in the
ovary, causes the stimulation of higher male hormones and leads to the
irregular periods and trouble getting pregnant. Progesterone is usually
missing—replacing it therefore makes sense. “
--------------------------------------------------------------------------------------------------------------
 John R Lee MD says: John R Lee MD says:
"I recommend supplementation of normal physiologic doses of progesterone
to treat PCOS. If progesterone levels rise each month during the luteal
phase of the cycle, as they are supposed to do, this maintains the
normal synchronal pattern each month, and PCOS rarely, if ever, occurs.
Natural progesterone should be the basis of PCOS treatment, along with
attention to stress, exercise, and nutrition.
If you have PCOS, you can use 15 to 20 mg of progesterone cream daily
from day 14 to day 28 of your cycle. If you have a longer or a shorter
cycle, adjust accordingly. The disappearance of facial hair and acne are
usually obvious signs that hormones are becoming balanced, but to see
these results, you'll need to give the treatment at least six months, in
conjunction with proper diet and exercise." This is quoted from the The John R Lee Medical Letter 1999.(10)
Self-Medication Not Recommended
Some young women find out about progesterone on internet messenger
boards, and then proceed on their own to buy it over-the-counter. The
progesterone cream may successfully restores cycles in many cases.
However, self - medication is not recommended. It is best to work with a
knowledgeable physician. If you have PCOS and need a doctor to
prescribe progesterone, you can find a knowledgeable physician on the ACAM or A4M doctor's directory.(65)(66) Always work closely with a knowledgeable physician.
Can PCOS be Treated with Natural Progesterone?
YES by Dr. Jerilynn Prior (3)
"Progesterone talks back to the hypothalamic and pituitary
(brain) hormones that control the ovaries and stops them from
stimulating the ovaries to make too much testosterone."
Dr Prior recognizes that the (BCP) pill, with its synthetic type of
progesterone, does help women with PCOS to a certain degree.
But her goal for PCOS patients is, "to return the brain/ovary system to a normal balance. The goal of the BCP Pill is the opposite - it must suppress the brain-ovary system to prevent pregnancy."
To help her PCOS patients achieve a normal hormonal balance, she prescribes oral micronized progesterone (trade
name Prometrium) which is a bio-identical hormone. Taking this natural
progesterone for two weeks every month (called cyclic progesterone
therapy) may help the brain to develop the normal cyclic rhythm that is
missing in PCOS.
Interestingly, Dr. Prior believes there is another benefit of cyclic
progesterone therapy. She explains, "most doctors don't realize
progesterone antagonizes and inhibits the enzyme (called 5-alpha
reductase) that is needed to make testosterone into dihydrotestosterone.
Dihydrotestosterone is the powerful male hormone that talks hair
follicles into making coarse hair and too much oil that causes acne."  Above quote is attributed to Jerilyn Prior MD Web Site.(3) Above quote is attributed to Jerilyn Prior MD Web Site.(3)
WHAT MAKES YOUR OVARIES TICK Insights about Ovulation, Fertility, PCOS and more. (4)
Click Here for an Interview
with Jerilynn C. Prior, M.D. posted on the Virgina Hopkins Health
Watch. Dr. Jerilynn Prior is a professor of endocrinology at the
University of British Columbia. She is a pioneer in research involving
women's menstrual cycles, ovulation, progesterone and bone loss.
___________________________________________________________________________________________
 Left Image: Polycystic ovary on ultrasound image. Left Image: Polycystic ovary on ultrasound image.
Interview Quoted from Virgina Hopkins Health Watch:
JLML: How do you track your luteal phase with a basal temperature chart?
JCPrior: If you record your oral temperature every morning for an entire
month using a digital thermometer, record the temperature in the
evening before you go to bed, and record any illness or early or late
rising, you can quantitatively determine which days of the cycle are
high progesterone days. You can then take all of those daily
temperatures from the beginning of one period until the day before the
beginning of the next, and do an average of the temperatures. The point
where your temperature goes above that average, and stays above it, is
the beginning of the luteal phase. It will go back down when your period
starts or just before. That's how easy it is to figure out your luteal
phase length! That alone is valuable information for women who are
having miscarriages that may be due to a short luteal phase.
JLML: I have found that women who are more aware of their cycles are often better able to self-treat for hormone imbalances.
JLML: What else can you tell us about anovulatory cycles? The other kind
of ovulation disturbance I called “turned on.” The woman experiencing
this kind of ovulation disturbance will complain of weight gain, acne,
and hair where she doesn’t want it. The biology of this is less clear,
but it relates to insulin excess and insulin resistance, which have
effects both on the brain by increasing LH (luteinizing hormone) levels,
and directly on the ovary. Excess insulin sits on receptors on the
theca cells, the outer coat of the ovary, and makes them more responsive
to the hormonal environment, and therefore they make more androgens
[testosterone, male hormones].
JLML: Aha! So that's why a high sugar diet aggravates polycystic ovary
syndrome. The excess sugar creates high insulin levels, which stimulate
androgen production in the ovary, which suppresses ovulation.
JCPrior: The higher LH and the higher androgen levels set up a signal
that inhibits the follicle from ovulating. Because each follicle grows
and creates a lake of fluid around it, if it doesn’t burst and release
its egg, a cyst is left. Therefore you get into a situation of high or
normal estrogen levels, high androgens, and low progesterone. That
condition is usually characterized by obesity, especially
middle-of-the-body obesity, androgen signs such acne, oily skin, facial
and breast hair, and head hair loss. Because estrogen tends to be higher
with weight gain, these are the women who have a higher breast cancer
and endometrial cancer risk. They may also have the worst PMS symptoms.
JLML: So this is yet another good reason to avoid sugar and refined carbohydrates such as white bread and pasta.
JCPrior: And it's another good reason to get plenty of aerobic or
endurance-type exercise, which is one of the best ways of getting the
insulin levels down and decreasing PMS. With turned on ovulation
disturbances you need to correct three problems: The first is to bring
progesterone into balance –and for this you use physiologic doses of
progesterone. Next, you often you need to block the effect of the male
hormone. There's a medicine called spironolactone which I use that
blocks androgen action at the cell level. Finally, if a person has a
family history of diabetes or is quite obese, then I may use a drug
called metformin (Glucophage) that sensitizes the body to insulin and
allows the insulin levels to go down.
JLML: I have found that supplemental progesterone, a good amount of exercise, and a low sugar diet, low simple carbohydrate and low fat diet with plenty of vegetables will often restore balance. The above interview posted courtesy of Virginia Hopkins Health Watch. (4)
Help for PCOS - Cyclic Progesterone Therapy
by Dr. Jerilynn C. Prior and Celeste Wincapaw (5)
Jerilynn C. Prior MD Says:
I use cyclic progesterone therapy as the heart of treatment for PCOS- anovulatory androgen excess.(6) Progesterone is the hormone made by the ovary after an egg is released.
The fundamental problem with PCOS is not making progesterone for two
weeks every cycle. This lack of progesterone leads to an imbalance in
the ovary, causes the stimulation of higher male hormones and leads to
the irregular periods and trouble getting pregnant. Progesterone is
usually missing—replacing it therefore makes sense. Progesterone talks
back to the hypothalamic and pituitary (brain) hormones that control the
ovary, and stops them from stimulating the ovary to make too much
testosterone.
Taking progesterone for two weeks every month (called cyclic
progesterone) may help the brain to develop the normal cyclic rhythm
that is missing in PCOS. Progesterone also counterbalances the steadily
high estrogen levels that the PCOS ovary produces even if you have no
periods. Progesterone will prevent estrogen over-stimulation of the
uterine lining (endometrial hyperplasia) and heavy flow. It may also
interfere with the action of high estrogen on the breasts, therefore
preventing tenderness and “lumpiness” and perhaps even the risk for
breast cancer.
Finally, and most doctors don’t realize this, progesterone antagonizes
and inhibits the enzyme (called 5-alpha reductase) that is needed to
make testosterone into dihydrotestosterone. Dihydrotestosterone is the
powerful male hormone that talks hair follicles into making coarse hair
and too much oil that causes acne.
 Useful Tools for Patients: Useful Tools for Patients:
Protocol for Cyclic PROGESTERONE THERAPY patient handout sheet (6)
Menstrual cycle diary log sheet patient handout (7) '
______________________________________________
Guidelines for Progesterone Cream Dosage for PCOS (8)
Early PCOS - 32mg from day 12-26
Advanced PCOS - 54mg from day 12-26 of your cycle
Severe PCOS with pain, 64mg of progesterone cream from
day 5-26 , to address pain from endometriosis. Then try to wean back to a
lesser dose or to extend breaks to fall into line with a day 12-26
cycle. Note, if you are using a regime day 5-26 in the first 4-7 months
until symptoms settle, please be aware you are using a program suggested
to enhance fertility. (8)
_______________________________________________
Dr. Lam Progesterone Guidelines for Polycystic Ovary Syndrome (9)
Dr. Lam follows Dr John R Lee pioneering use of progesterone.
Apply 20 mg of progesterone cream during day 14 to 28 of the menstrual
cycle. Adjust accordingly if for longer or shorter cycle. As the
hormonal balance is regained, facial hair and acne, two commonly
associated symptoms, will disappear. (9)
_______________________________________________
Other treatable causes of anovulation
1) Low thyroid function (hypothyroid) causes menstrual
irregularity, anovulation and infertility. Ovulation and fertility is
restored by thyroid medication. Ovarian cysts also resolve.
2) Vitamin D deficiency is associated with anovulation. Resolves with Vitamin D.
3) Iodine deficiency causes ovarian cysts and anovulation, reversed by iodine supplementation.
________________________________________________
Other Useful Drug Treatments for PCOS:
Issue Drug Treatment
Infertility, anovulation: Clomid clomephine, induces ovulation.
Insulin Resistance: Metformin improves insulin sensitivity.(39)(39A)
Acne, Facial Hair: Spironlactone, Aldactone inhibits testosterone.
________________________________________________
PCOS—polycystic ovary syndrome.
Standard diagnostic assessments:
1) History may show: Variable or anovulatory menstrual pattern, obesity, hirsutism, and the absence of breast discharge.
2) Pelvic sonogram may show: 10 or more cysts in each ovary, 'string of pearls'.
The ovaries are generally 1.5 to 3 times larger than normal.
3) Labs may show:
Elevated DHEAs and free testosterone.
Ratio of LH to FSH is greater than 1:1, as tested on Day 3 of the menstrual cycle.
The pattern is not very specific and was present in less than 50% in one study.
Common assessments for associated conditions or risks.
1) Fasting biochemical screen and lipid profile
2) 2-hour oral glucose tolerance test (GTT) in patients with risk
factors (obesity, family history, history of gestational diabetes) and
may indicate impaired glucose tolerance (insulin resistance) in 15-30%
of women with PCOS. Frank diabetes can be seen in 65–68% of women with
this condition. Insulin resistance can be observed in both normal weight
and overweight patients.
Lab tests for exclusion of other disorders that may cause similar symptoms:
1) Prolactin
2) TSH
3) 17-hydroxyprogesterone to rule out 21-hydroxylase deficiency (CAH).
4) Fasting insulin level or GTT with insulin levels (also called IGTT).
5) Fasting Glucose to Fasting Insulin ratio <4.5 is cheaper method
ICD-9 Codes: PCOS ICD-9 256.4 Amenorrhea ICD-9 626.0
___________________________________________
Non Classical CAH Congenital Adrenal Hyperplasia, also known as Non-Classical 21 Hydroxylase Deficiency (NC21OHD)
Non-Classical CAH or 21 Hydroxylase Deficiency is the most common
genetic disease known, occurring in 1% of New Yorkers, and up to 3% in
ethnic groups such as of Ashkenazi Jews, Hispanics, Italians, and
Yugoslavs.(68)
Ten per cent of patients with PCOS actually have Non-Classical CAH. The
underlying genetic defect causes an enzyme deficiency in the adrenal
gland which reduces the ability of the adrenal to make
cortisol. Instead of making cortisol, the adrenal steroid pathways are
shunted towards testosterone causing elevated testosterone and the
typical symptoms of hair growth (hirsutism), and acne and there may also
be menstrual irregularities, anovulation, and infertility.(69)(70)
What is the 21 Hydroxylase Enzyme?
This is a key enzyme in the adrenal gland which converts cholesterol
into cortisol. In the Classical form of CAH, the 21 hydroxylase enzyme
(21-OH) is severely deficient with resulting low cortisol levels. In
the Non-Classical form however, the 21 hydroxylase (21-OH) enzyme is
still working fairy well with only a slight reduction in activity, and
cortisol levels are usually normal, while testosterone levels may be
elevated to a variable degree. The Human Adrenal Steroid synthesis
pathways and the adrenal enzymes involved can be understood on this chart from Quest Labs.(71)
How to Make the Diagnosis of Non-Classical CAH? Cortrosyn Stimulation
The most definitive diagnosis is done with a Cortrosyn Stimulation test
(0.25 mg) which measures 17-hydroxyprogesterone (17-OHP) at 0 and 60
minutes after SQ injection of the Cortrosyn (ACTH).
This test in simple terms is described here:
First a preliminary (baseline ) blood test is done for various hormones
including 17-OH, this is followed by a subcutaneous injection of 0.25 mg
of a drug called Cortrosyn which is a form of ACTH which stimulates the
adrenal glands to make more hormones. An hour (60 minutes) after the
Cortrosyn injection, a post stimulation blood sample is drawn for lab
testing for 17-OH and other hormones.
Patients with Non Classic 21-OH Deficiency typically show 60-min stimulated 17-OHP values between 1,500 and 10,000 ng/dl. This chart
shows how the 17-OHP values cluster at three areas for normal (below
1,500), Non-Classical CAH (1500-10,000) and, and Classical CAH (above
10,000). (72) The Quest Lab testing algorithm is shown here.(73)
Genetic Testing for 21-OH Deficiency
Genetic testing is now available and very useful. This test shows
whether or not there is a mutation in the CYP21A2 gene coding for the
21-Hydroxylase Enzyme.(74) The CAHDtex test by Esoterix is useful in showing the exact mutation in the CYP21A2 gene. (75) Once the exact mutation in the CYP21A2 gene is known, refer to this chart to determine the severity of the enzyme defect.(76) Genetic testing of other family members is usually recommended once a sibling is found with the mutation.
Clinical Presentation in Children
In children, the signs include premature onset of puberty, cystic acne,
accelerated growth, and advanced bone age. Premature development of
pubic hair may occur as early as 6 months of age (due to elevated
testosterone). The severe cystic acne may be unresponsive to oral
antibiotics and retinoic acid (Accutane).
Although the child may be taller than the other kids in early childhood,
this early growth spurt finishes early (because of epiphyseal fusion),
and final height ends up shorter than usual. Thus, these kids are tall
children but short adults.
Another feature may be male pattern baldness in a female involving the top of the head and sparing the sides.
Teenagers and Young Adults - Major Cause of Infertility
Teenage girls may present with features of elevated testosterone such as
facial hair (hirsutism), acne and menstrual irregularities or
anovulation. Young adult females may present with the chief complaint of
infertility. It has been generally recognized that infertility of
undetermined cause in women may be reversed with glucocorticoid (cortef
or prednisone) therapy, which most likely treats an occult Non-Classical
CAH Syndrome. William Mc Jefferies MD successfully treated thousands
of such cases ( The Safe Uses of Cortisol).(77)
Treatment of Non Classical CAH with Cortisol Restores Fertility
Oral tablets containing low dose cortisol sucessfully treat
Non-Classical CAH and reverse the symptoms restoring fertility. The
cortisol suppresses ACTH and reduces the testosterone production by the
adrenal.
Dr. Maria New has followed a large group of 400 patients with
Non-Classical CAH, and she treats them with 0.25 mg dexamethasone at the
hour of sleep, and she notes it takes about 3 months for reversal of
acne and infertility. Hirsutism takes longer to respond, about 30
months.
The cost for a dexamethasone tablet is $0.50, and the 3-month treatment
cost is estimated to be $45. Compare this $45 dollars to the infertility
treatment cost of $30,000 for one cycle of in vitro fertilization . Dr.
Maria New says that many patients presenting with infertility actually
have NonClassical CAH, and fertility could be restored
easily with treatment with oral cortisol tablets such as cortef,
dexamethasone, or prednisone. (69)
Before you spend a fortune on in-vitro fertilization for infertility,
it would be prudent to rule out Non-Classical CAH with a simple genetic
test. For more information on CAH, see : A Commonly Missed Cause of Infertility, NonClassical CAH by Jeffrey Dach MD (78)
Articles with Related Interest
PCOS Part Two
PCOS Part three
Jeffrey Dach MD
7450 Griffin Rd Suite 180/190
Davie, FL 33314
Phone: 954-792-4663
Facebook
Blog
REFERENCES
(1) http://www.amazon.com/Clinical-Gynecologic-Endocrinology-Infertility-Editorial/dp/0781747953
The Clinical Gynecologic Endocrinology and Infertility: Leon Speroff MD
(2) http://jcem.endojournals.org/cgi/content/full/88/5/1927
A Modern Medical Quandary: Polycystic Ovary Syndrome, Insulin Resistance, and Oral Contraceptive Pills, The Journal of Clinical Endocrinology & Metabolism Vol. 88, No. 5 1927-1932
(3) http://www.pcosupport.org/newsletter/articles/article122707-3.php
Can PCOS be Treated with Natural Progesterone? Jerilynn Prior, PCOSA Today Newsletter
(4) http://www.virginiahopkinstestkits.com/priorovaries.html
WHAT MAKES YOUR OVARIES TICK, Insights about ovulation, fertility, PCOS
and more.An Interview with Jerilynn C. Prior, M.D. FRCPC
(5) http://www.cemcor.ubc.ca/help_yourself/articles/challenge_pcos
Help for Anovulatory Androgen Excess (AAE)—Challenge PCOS! by Dr. Jerilynn C. Prior and Celeste Wincapaw
(6) http://www.cemcor.ubc.ca/files/uploads/Cyclic_Progesterone_Therapy.pdf
INFORMATION FOR WOMEN: CYCLIC PROGESTERONE THERAPY Protocol for treatment.
(7) http://www.cemcor.ubc.ca/files/uploads/Menstrual_Cycle_Diary_with_treatments.pdf
Menstrual Cycle Diary / Log Book / Calendar
(8) http://www.natural-progesterone-advisory-network.com/
what-is-the-guidelines-to-progesterone-dosage/
What is the guidelines to progesterone dosage for PCOS ? National Progesterone Advisory Network
(9) http://www.drlam.com/A3R_brief_in_doc_format/progesterone.cfm
Dr. Lam Progesterone Page
(10) http://www.virginiahopkinstestkits.com/pcos.html
What Your Dr. May Not Tell You about PCOS, Polycystic Ovary Syndrome
(PCOS), A New Epidemic that Causes Infertility, Excess Hair, Acne and
More By John R. Lee, M.D. and Virginia Hopkins
(11) http://www.townsendletter.com/Nov2004/phyto1104.htm
Townsend Letter, Phytotherapy for Polycystic Ovarian Syndrome (PCOS) by
Angela Hywood N.D. & Kerry Bone, Townsend Letter message Boards
(12) http://pcos.meetup.com/217/
PCOS GROUPS and Message Boards, The Arizona Polycystic Ovarian Syndrome Meetup Group,
(13) http://search.yahoo.com/
search?p=pcos+message+board&fr=yfp-t-501-s&toggle=1&cop=mss&ei=UTF-8
Hundreds of PCOS Message Boards
(14) http://www.early-pregnancy-tests.com/vitex.html
Home Ovulation Tests, Pregnancy Test Kits, Basal Thermometers
Birth Control Pills
(15) http://www.sensible-alternative.com.au/polycystic_ovarian_syndrome.html
The Birth Control Pill is NOT the Answer. The birth control pill does
absolutely nothing to improve insulin resistance, and can actually
worsen it
(1). “They may, however, worsen insulin resistance and lead to
deterioration of glucose tolerance.” Glucose tolerance deteriorated
significantly, and two women developed diabetes” In 2003, the Journal of
Clinical Endocrinology & Metabolism published an article called 'A
Modern Medical Quandary: Polycystic Ovary Syndrome, Insulin Resistance,
and Oral Contraceptive Pills'.
(2) The Pill has been standard treatment for PCOS, and yet, perversely,
it appears to worsen the metabolic problem that is at the root of the
condition. The authors say:
'...what has been lacking is a critical examination of whether oral
contraceptives might...exert adverse metabolic effects with long-term
consequences..'.
I propose that the Pill has made additional contributions to the
epidemic of PCOS. The Pill is known to cause permanent hormone changes,
even once it is stopped.
(3). Most doctors agree that it can take 1 to 2 years for normal
menstrual cycles to resume after stopping the pill . The pill will cause
a monthly bleed, but this is not a true period.
(16) http://jcem.endojournals.org/cgi/content/full/82/9/3074
The Journal of Clinical Endocrinology & Metabolism Vol. 82, No. 9
3074-3077. The Effect of a Desogestrel-Containing Oral Contraceptive on
Glucose Tolerance and Leptin Concentrations in Hyperandrogenic Women
Shahla Nader, Maggy G. Riad-Gabriel and Mohammed F. Saad
(17) http://jcem.endojournals.org/cgi/content/full/88/5/1927
Diamanti-Kandarakis, E et al. A modern medical quandary: Polycystic
Ovary Syndrome, Insulin Resistance, and Oral Contraceptive Pills. J Clin
End Met 2003.88(5): 1927-1932 CONTROVERSIES IN ENDOCRINOLOGY Evanthia
Diamanti-Kandarakis, Jean-Patrice Baillargeon, Maria J. Iuorno, Daniela
J. Jakubowicz and John E. Nestler
(18) http://www.ncbi.nlm.nih.gov/pubmed/16409223
Panzer et al. Impact of Oral Contraceptives on Sex Hormone-Binding
Globulin and Androgen Levels: A Retrospective Study in Women with Sexual
Dysfunction. The Journal of Sexual Medicine. 2006. 3:p.104-113
(19) http://www.eurekalert.org/pub_releases/2006-01/bpl-ocp121305.php
Birth Control Pill Side effects. Oral contraceptive pill may prevent more than pregnancy
New research indicates birth control pill could cause long-term problems with testosterone
(20) http://ditchthepill.org/
Ditch the Pill . org, very neative about BCPs
Jones, M.D. Medical Director, Women’s Health Institute
THYROID References
(21) http://www.ncbi.nlm.nih.gov/pubmed/16208308?dopt
Abstract Minerva Endocrinol. 2005 Sep;30(3):193-7. Relationship between
insulin secretion, and thyroid and ovary function in patients suffering
from polycystic ovary. CONCLUSIONS: The data obtained in our study
enable us to support the close connection between ovary function,
thyroid function and insulin-resistance. In all patients, in fact,
albeit at different times, an improvement was obtained in all 3
pathologies.
(22) http://www.ncbi.nlm.nih.gov/pubmed/17302862
Thyroid disease and female reproduction. Poppe K, Velkeniers B, Glinoer D. Clin Endocrinol (Oxf). 2007 Mar;66(3):309-21
(23) http://www.ncbi.nlm.nih.gov/pubmed/15012623
High prevalence of autoimmune thyroiditis in patients with
polycystic ovary syndrome.Janssen OE. Eur J Endocrinol. 2004
Mar;150(3):363-9. CONCLUSION: This prospective study demonstrates a
threefold higher prevalence of Autoimmune Thyroid disorders in patients
with PCOS
Prevalence of PCOS in Population
(24) http://jcem.endojournals.org/cgi/content/full/85/7/2434
A Prospective Study of the Prevalence of the Polycystic Ovary Syndrome
in Unselected Caucasian Women from Spain. Our results demonstrate a 6.5%
prevalence of PCOS, as defined, in a minimally biased population of
Caucasian women from Spain. The polycystic ovary syndrome, hirsutism,
and acne are common endocrine disorders in women. The Journal of
Clinical Endocrinology & Metabolism Vol. 85, No. 7 2434-2438
Thyroid References
(25) http://www.ncbi.nlm.nih.gov/pubmed/8053991
Hypothyroidism presenting with polycystic ovary syndrome.Sridhar GR.
J Assoc Physicians India. 1993 Feb;41(2):88-90. During a 30 months
period, two women of primary hypothyroidism (2/13; 1.04%) presented with
features of polycystic ovary syndrome (PCOS). In hypothyroidism, sex
hormone binding globulin levels are decreased; increased conversion of
androstenedione to testosterone, and aromatization to estradiol are
present, all these being an exaggeration of biochemical changes
characteristic of PCOS. Besides, metabolic clearance rates of
androstenedione and estrone, the putative mediators of PCOS, are
reduced. Hypothyroidism can either initiate, maintain or worsen the
syndrome. Correction of hypothyroidism when present, would therefore
form an important aspect in the management of infertility associated
with PCOS.
(26) http://www.ncbi.nlm.nih.gov/pubmed/17954423
Precocious puberty and large multicystic ovaries in young girls with
primary hypothyroidism.Sanjeevaiah AR, Sanjay S, Deepak T, Sharada A,
Srikanta SS. Samatvam Endocrinology Diabetes Center, Bangalore, India.
(27) http://www.ncbi.nlm.nih.gov/pubmed/17917634
Mymensingh Med J. 2007 Jul;16(2 Suppl):S60-62. Vaginal bleeding with
multicystic ovaries and a pituitary mass in a child with severe
hypothyroidism.Mohsin F, Nahar N, Azad K, Nahar J. Department of
Paediatrics, Bangladesh Institute of Research and Rehabilitation on
Diabetes, Endocrine and Metabolic Disorders (BIRDEM), Dhaka, Bangladesh.
A seven year and ten months old girl presented with cyclic vaginal
bleeding and a huge abdominopelvic mass. She had clinical features of
hypothyroidism. The investigation results were consistent with the
diagnosis of primary hypothyroidism with precocious puberty. She also
had bilaterally enlarged cystic ovaries on CT scan of abdomen and CT
scan of brain showed pituitary macroadenoma. After starting treatment
with thyroxine, patient became euthyroid and her general condition
improved. Treatment with thyroxine alone halted the cyclic vaginal
bleeding, led to rapid resolution of the ovarian cysts and regression of
the pituitary mass.
(28) http://www.ncbi.nlm.nih.gov/pubmed/2729396
Spontaneous ovarian hyperstimulation syndrome associated with
hypothyroidism. Rotmensch S, Scommegna A. Department of Obstetrics and
Gynecology, Michael Reese Hospital and Medical Center, University of
Chicago, Pritzker School of Medicine, IL 60616. Am J Obstet Gynecol.
1989 May;160(5 Pt 1):1220-2.
(29) http://www.ncbi.nlm.nih.gov/pubmed/17954423?ordinalpos=4&itool=EntrezSystem2.PEntrez.Pubmed.Pubmed_ResultsPanel.Pubmed_RVDocSum
Precocious puberty and large multicystic ovaries in young girls with
primary hypothyroidism.Sanjeevaiah AR, Sanjay S, Deepak T, Sharada A,
Srikanta SS. Endocr Pract. 2007 Oct;13(6):652-5.
(30) http://www.ncbi.nlm.nih.gov/pubmed/16864150
Primary hypothyroidism presenting as ovarian tumor and precocious
puberty in a prepubertal girl.Campaner AB, Scapinelli A, Machado RO, Dos
Santos RE, Beznos GW, Aoki T. Department of Obstetrics and Gynecology,
Santa Casa São Paulo-Faculty of Medical Science, São Paulo, Brazil.
Gynecol Endocrinol. 2006 Jul;22(7):395-8.
We report a case of a prepubertal girl with juvenile primary
hypothyroidism presenting as ovarian cysts and precocious puberty. The
7-year-old female was referred to our clinic because of a
pelvic/abdominal mass and vaginal bleeding. Besides these findings, on
physical examination we noticed the thyroid gland globally increased and
the presence of secondary sexual characteristics. Based upon the
clinical profile and investigations, the patient was diagnosed with
juvenile primary hypothyroidism due to autoimmune thyroiditis. The cysts
and precocious puberty resolved spontaneously after the simple
replacement of thyroid hormone. It is important to bear in mind
hypothyroidism in cases of girls presenting ovarian cysts and precocious
puberty in order to avoid unnecessary surgery on the ovaries.
(31) http://www.ncbi.nlm.nih.gov/pubmed/16995569
J Pediatr Endocrinol Metab. 2006 Jul;19(7):895-900.
Ovarian cysts in young girls with hypothyroidism: follow-up and effect
of treatment.Sharma Y, Bajpai A, Mittal S, Ovarian cysts have been
reported in girls with longstanding uncompensated primary
hypothyroidism. Restoration of euthyroid state has been associated with
resolution of these cysts; long-term follow-up of these patients is
however lacking. Our study emphasizes the need to exclude
hypothyroidism in young girls with ovarian cysts. A causal link between
hypothyroidism and spontaneously occurring ovarian hyperstimulation
syndrome is suggested by analysis of data from a patient with myxedema
and review of data from animal research.
(32) http://www.jacemedical.com/articles/Sub-laboratory%20Hypothyroidism%20.pdf
“Sub-laboratory” Hypothyroidism and the Empirical use of Armour® Thyroid
Alan R. Gaby, MD . Excellent revierw on subclinical hypothyroidism.
"Of 12 girls (ages 9-16) with severe and longstanding hypothyroidism,
nine were diagnosed by pelvic ultrasound with PCOS. The cysts resolved
rapidly after treatment with thyroid hormone. In another study of
hypothyroid patients with PCOS, administration of thyroid hormone was
associated with normalization of ovulation.23 These observations raise
the possibility that sublaboratory hypothyroidism is a contributing
factor in some cases of PCOS."
Lindsay AN, Voorhess ML, MacGillivray MH. Multicystic ovaries in primary hypothyroidism.Obstet Gynecol 1983;61:433-437. 23.
Ghosh S, Kabir SN, Pakrashi A, et al. Subclinicalhypothyroidism: a determinant of polycystic ovary syndrome.
Iodine and PCOS
(33) http://www.optimox.com/pics/Iodine/pdfs/IOD02.pdf
Orthoiodosupplementation: Iodine sufficiency of the whole human Guy. E.
Abraham M.D.1, Jorge D. Flechas M.D.2 and John C. Hakala R.Ph.Our
preliminary experience with I supplementation at 12.5 mg/day. Our
findings in 3 patients with Polycystic Ovarian Syndrome (PCOS) confirmed
the positive response observed following supplementation with 10 to 20
mg of potassium iodide by Russian investigators 40 years ago (62). Prior
to I supplementation, those PCOS patients were olygomenorrheic,
menstruating one or twice a year. Following I supplementation for 3
months, they resumed normal monthly cycles.
(34) http://optimox.com/pics/Iodine/opt_Research_I.shtml
Listing of Iodine publications at the Optimox Web Site.
(35) http://optimox.com/pics/Iodine/IOD-10/IOD_10.htm
Orthoiodosupplementation in a Primary Care Practice Jorge D. Flechas, M.D.
Iodine deficiency may cause the ovaries to develop cysts , nodules and
scar tissue. At its worse this ovarian pathology is very similar to that
of polycystic ovarian syndrome (PCOS). As of the writing of this
article I have five PCOS patients. The patients have successfully been
brought under control with the use of 50 mg of iodine per day. Control
with these patients meaning cysts are gone, periods every 28 days and
type 2 diabetes mellitus under control.
(36) http://cypress.he.net/~bigmacnc/drflechas/index.htm
HelpMyThyroid, George Flechas MD web site
Vitamin D and PCOS
(37) http://www.ncbi.nlm.nih.gov/pubmed/17177140
Low serum 25-hydroxyvitamin D concentrations are associated with
insulin resistance and obesity in women with polycystic ovary syndrome.
Exp Clin Endocrinol Diabetes. 2006 Nov;114(10):577-83. Hahn S et
al. Insulin resistance (IR) and central obesity are common features of
the polycystic ovary syndrome (PCOS). Vitamin D is thought to play a
role in the pathogenesis of type 2 diabetes by affecting insulin
metabolism. Subgroup analysis of lean, overweight and obese women
revealed significant higher 25-OH-VD levels in lean women. Differences
remained significant when women were divided according to their 25-OH-VD
levels. Women with hypovitaminosis D (<9 ng/ml) had higher mean BMI,
indices of IR and leptin levels compared to women with normal serum
levels (all p<0.05). Analysis of vitamin D and biochemical endocrine
PCOS features revealed a significant correlation only between 25-OH-VD
and sex hormone-binding globulin as well as the free androgen index. In
conclusion, in PCOS women, low 25-OH-VD levels are associated with
obesity and insulin resistance .
(38) http://www.ncbi.nlm.nih.gov/pubmed/10433180
Vitamin D and calcium dysregulation in the polycystic ovarian
syndrome.Thys-Jacobs S, Donovan D, Papadopoulos A, Sarrel P, Bilezikian
JP. Department of Medicine, St. Lukes-Roosevelt Hospital Center,
Columbia University, College of Physicians & Surgeons, New York, NY
10019, USA. Steroids. 1999 Jun;64(6):430-5.
Over the past 30 years, numerous studies in invertebrates and
vertebrates have established a role of calcium in oocyte maturation as
well as in the resumption and progression of follicular development.
Polycystic ovarian syndrome (PCO) is characterized by hyperandrogenic
chronic anovulation, theca cell hyperplasia, and arrested follicular
development. The aim of this observational study was to determine
whether vitamin D and calcium dysregulation contribute to the
development of follicular arrest in women with PCO, resulting in
reproductive and menstrual dysfunction. Thirteen premenopausal women
(mean age 31 +/- 7.9 years) with documented chronic anovulation and
hyperandrogenism were evaluated. Four women were amenorrheic and nine
had a history oligomenorrhea, two of whom had dysfunctional bleeding.
Nine had abnormal pelvic sonograms with multiple ovarian follicular
cysts. All were hirsute, two had alopecia, and five had acanthosis
nigricans. The mean 25 hydrovitamin D was 11.2 +/- 6.9 ng/ml [normal
(nl): 9-52], and the mean 1,25 dihydroxyvitamin D was 45.8 +/- 18 pg/ml.
with one woman with a 1,25 dihydroxyvitamin D <5 pg/ml (nl: 15-60).
The mean intact parathyroid hormone level was 47 +/- 19 pg/ml (nl:
10-65), with five women with abnormally elevated parathyroid hormone
levels. All were normocalcemic (9.3 +/- 0.4 mg/dl).
Vitamin D repletion with calcium therapy resulted in normalized menstrual cycles within 2 months for seven women,
with two experiencing resolution of their dysfunctional bleeding. Two
became pregnant, and the other four patients maintained normal menstrual
cycles. These data suggest that abnormalities in calcium homeostasis
may be responsible, in part, for the arrested follicular development in
women with PCO and may contribute to the pathogenesis of PCO.
METFORMIN
(39) http://content.nejm.org/cgi/content/extract/358/1/47
Metformin for the Treatment of the Polycystic Ovary Syndrome John E.
Nestler, M.D. N. Engl. J. Med., January 3, 2008; 358(1): 47 - 54.
(39A) http://www.ovarian-cysts-pcos.com/glucophage-metformin-pcos.html
PCOS and Metformin (Glucophage)
Diet and Weight Loss
(40) http://www.ovarian-cysts-pcos.com/pcos-book-res.html
The Natural Diet Solution for PCOS and Infertility Nancy Dunne, ND Bill Slater, MBA
(41) http://www.ovarian-cysts-pcos.com/PCOS-success.html#sec1
PCOS success stories by Nancy Dunne
Conventional Medical Diagnosis and Treatment of PCOS
(42) http://www.amazon.com/Clinical-Gynecologic-Endocrinology-Infertility-Editorial/dp/0781747953
Speroff on PCOS: Clinical Gynecologic Endocrinology and Infertility by Leon Speroff MD p.493
“A question which has puzzled gynecologists and endocrinologists for
many years is what causes polycystic ovaries. There is an answer which
is appealing in its logic and clinical applicability. The characteristic
polycystic ovary emerges when a state of anovulation persists for any
length of time” Should you have a sonogram to make the diagnosis of
PCOS? “From 8-14% of normal women will demonstrate ultrasonographic
findings typical of polycystic ovaries. Ultrasonography as a diagnostic
tool for this condition is unnecessary, and we vigorously discourage its
use for this purpose.”
(43) http://assets.cambridge.org/97805218/48497/excerpt/9780521848497_excerpt.pdf
Exerpt from Book: Introduction: Polycystic ovary syndrome is an
intergenerational problem. Gabor T. Kovacs and Robert Norman Cambridge
University Press 978-0-521-84849-7 - Polycystic Ovary Syndrome, Second
Edition
(44) http://findarticles.com/p/articles/mi_qa3890/is_200407/ai_n9457295/pg_1
Hoyt, Karri Lynn "Polycystic Ovary (Stein-Leventhal) Syndrome: Etiology,
Complications, and Treatment". Clinical Laboratory Science. Summer
2004.
(45) http://health.nytimes.com/health/guides/disease/polycystic-ovary-disease/overview.html
Polycystic Ovary Disease article in the New York Times
(46) http://www.ebmonline.org/cgi/content/full/229/5/369
MINIREVIEW, Screening for and Treatment of Polycystic Ovary Syndrome in Teenagers.
Experimental Biology and Medicine 229:369-377 (2004) Darren J. Salmi et al.
(47) http://www.drgalen.com/pcos.html
Dr. Galen, Reproductive Science Centerª of the San Francisco Bay Area,
POLYCYSTIC OVARY SYNDROME (PCOS) Treatment of PCOS: In cases where
ovulation is irregular or absent, medication can be used. The most
common agent is clomiphene citrate (Clomid, Serophene), which is
generally taken daily from days 3-7 of a cycle. Ovarian follicle
development is usually monitored with a combination of home urinary LH
testing, and office ultrasound examination. An intrauterine insemination
is frequently advised because of clomiphene's adverse effect on a
womanÕs cervical mucous quality. Additional endometrial support may be
promoted with the use of progesterone or HCG injections. There is a
mildly increased rate of multiple pregnancy with clomiphene (6-7%) but
there is no increased risk of birth defects. The majority of womn who
conceive on clomiphene will do so in the first 4 cycles. If clomiphene
fails to successfully induce ovulation and/or pregnancy, then a group of
injectable hormone preparations, known as gonadotropins, may be
employed.
(48) http://www.clinmedres.org/cgi/content/full/2/1/13
Clinical Medicine & Research Volume 2, Number 1 : 13 -27, 2004,
Polycystic Ovarian Syndrome: Diagnosis and Management Michael T.
Sheehan, MD. Marshfield Clinic. Excellent review of conventional
diagnosis and treatment for PCOS.
(49) http://www.inciid.org/printpage.php?cat=pcos&id=505
Understanding and managing Polycystic Ovarian Syndrome (PCOS) by Sam
Thatcher, M.D., Ph.D. director of the Center for Applied Reproductive
Science in Johnson City, TN,. Conventional Approach.
(50) http://www.perspectivespress.com/0-944934-25-0.html
PCOS: The Hidden Epidemic. a Book by Sam Thatcher MD PhD, Conventional Approach to PCOS.
(51) http://www.emedicine.com/ped/topic2155.htm
Polycystic Ovarian Syndrome Last Updated: September 15, 2006, on E-Medicine.
(52) http://www.endotext.org/female/female6/female6.htm
ENDOTEXT.COM, HYPERANDROGENISM, HIRSUTISM AND POLYCYSTIC OVARY
SYNDROMEChapter 6 - Randall B. Barnes, M.D., Adrienne B. Neithardt, M.D.
and Suleena K. Kalra, M.D.November 19, 2003 on Endotext.com
(53) http://jcem.endojournals.org/cgi/content/full/89/2/453
EXTENSIVE PERSONAL EXPERIENCE Androgen Excess in Women: Experience with
Over 1000 Consecutive Patients R. AZZIZ, L. A. SANCHEZ, E. S.
KNOCHENHAUER, C. MORAN, J. LAZENBY, K. C. STEPHENS,K. TAYLOR, AND L. R.
BOOTS The Journal of Clinical Endocrinology & Metabolism
89(2):453–462. All patients with menstrual or ovulatory dysfunction
received BCPs' (OCs) when possible. Patients with unwanted hair growth
and evidence of excess facial or body terminal hair growth received
spironolactone (SPA) (200 mg ; 100 mg/d) in combination with the OC, to
minimize the risks of teratogenicity. SPA was rarely used alone, except
in the occasional hirsute patient who had previously undergone a
hysterectomy or tubal ligation. Other treatment regimens were
occasionally used, including glucocorticoids, insulin sensitizers, GnRH
analogs, flutamide, finasteride, and other estrogen-progestin
combinations, alone or in combination; the majority of these were used
as part of clinical trials (24–26).
(54) http://www.joplink.net/prev/200201/ref/01-02.html
Stein IF, Leventhal ML. Amenorrhoea associated with bilateral polycystic ovaries. Am J Obstet Gynecol 1935;29:181–91.
The Environment, Endocrine Disruptor Chemicals and PCOS
(55) http://www.ourstolenfuture.org/Consensus/2005/2005-1030vallombrosa.htm
Vallombrosa Consensus Statement on Environmental contaminants and human fertility compromise.
October 2005.
(56) http://www.ourstolenfuture.org/index.htm
Our Stolen Future, endocrine disruptors in the environment
(57) http://www.ovarian-cysts-pcos.com/news13-pcos-pesticides.html#sec1
Pesticides and PCOS
(58) http://humupd.oxfordjournals.org/cgi/reprint/7/3/323.pdf
Endocrine Disruptors as environmental cause of PCOSThe impact of
Endocrine Disruptors on the Female Reproductive System, Stamati and
pitsos et al.
Testosterone for Women
(59) http://www.asrm.org/Literature/Menopausal_Medicine/menomedsummer01.pdf
Testosterone Treatment: Psychological and Physical Effects in Postmenopausal Women.
Susan R. Davis, M.B.B.S., F.R.A.C.P., Ph.D. Menopausal Volume 9, Number 2, Summer 2001
Diet for PCOS
(61) http://pcos.is/files/pcosbook1.pdf
A complete online book on Diet and Nutrition for PCOS by Nancy Dunn
(62) http://www.topfitonline.com/chartglycemic.htm
Glycemic Index Chart - handy and useful.
Questionnaire for PCOS
(63) http://www.cfp.ca/cgi/content/full/53/6/1041/T50531041
Table 5 Clinical tool for diagnosis of polycystic ovary syndrome
Can Fam Physician Vol. 53, No. 6, June 2007, pp.1041 - 1047 , Polycystic
ovary syndrome. Validated questionnaire for use in diagnosis, Sue D.
Pedersen, et al.
(64) http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1949220
Can Fam Physician. 2007 June; 53(6): 1041–1047. Polycystic ovary
syndrome. Validated questionnaire for use in diagnosis, Sue D. Pedersen,
et al.
(65)http://www.acamnet.org/site/c.ltJWJ4MPIwE/b.2242497/k.2C78/Integrative_Medicine_
Physicians/apps/kb/cs/contactsearch.asp
ACAM doctor's directory
(66) http://www.worldhealth.net/pages/directory
A4M doctor's directory
(67) http://jeffreydach.com/2008/02/27/a-commonly-missed-cause-of-infertility-nonclassical-cah-by-jeffrey-dach-md.aspx A Commonly Missed Cause of Infertility, NonClassical CAH by Jeffrey Dach MD
Non Classical Adrenal Hyperplasia CAH 21-OH Deficiency
(68) http://jcem.endojournals.org/cgi/content-nw/full/91/11/4205/F8
FIG. 8. Non-classical CAH 21 Hydroxylase Deficiency Chart of Disease frequencies in different ethnic groups.
(69) http://jcem.endojournals.org/cgi/content/full/91/11/4205
The Journal of Clinical Endocrinology & Metabolism Vol. 91, No. 11 4205-4214
EXTENSIVE CLINICAL EXPERIENCE, Nonclassical 21-Hydroxylase Deficiency
Maria I. New Department of Pediatrics, Mount Sinai School of Medicine, New York, New York 10029
(70) http://www.mcg.edu/pediatrics/pedsendo/21.pdf
Consensus Statement on Treatment of 21-Hydroxylase Deficiency. JCEM 87(9):4048-4053, 2002.
(71) http://www.questdiagnostics.com/hcp/intguide/EndoMetab/Gen_Misc/TG_CAH/TG_CAH_Fig1.pdf
Chart showing pathways of steroid synthsis Quest LAbs.
(72)http://jcem.endojournals.org/cgi/content/full/91/11/4205/F5
FIG. 5. Nomogram relating baseline to ACTH-stimulated serum
concentrations of 17-OHP. The scales are logarithmic. A regression line
for all data points is shown.
(73)
http://www.questdiagnostics.com/hcp/intguide/jsp/showintguidepage.jsp?fn=EndoMetab/Gen_Misc/TG_CAH/TG_CAH.htm
Congenital Adrenal Hyperplasia Testing Algorithm Guide Quest LAbs
(74) http://www.questdiagnostics.com/hcp/intguide/EndoMetab/EndoManual_AtoZ_PDFs/CAH_Common.pdf
21 Hydroxylase Deficiency Common Mutations, Quest LAbs
(75) http://www.esoterix.com/files/ss_cah.pdf
DNA TESTING FOR 21-HYDROXYLASE DEFICIENCY, Esoterix introduces a new DNA
test to identify deficiency in the 21-hydroxylase gene, the most common
cause of congenital adrenal hyperplasia (CAH). CAHDetx evaluates
the CYP21 gene, detecting mutations and gene deletion/conversions that
account for approximately 90% to 95% of all CAH cases.
(76) http://jcem.endojournals.org/cgi/content-nw/full/91/11/4205/T1
TABLE 1. Common gene mutations of the 21-hydroxylase gene CYP21A2 (75 )
(77) http://www.amazon.com/review/R2IPB7XGMO20NE/ref=cm_cr_rdp_perm
Safe Use of Cortisol is a Unique Medical Classic, December 7, 2007 By Jeffrey Dach MD
(78) A Commonly Missed Cause of Infertility, NonClassical CAH by Jeffrey Dach MD
Jeffrey Dach MD
7450 Griffin Road Suite 190
Davie, Florida 33314
954-792-4663
http://www.drdach.com/
http://www.naturalmedicine101.com/
http://www.truemedmd.com/
http://www.bioidenticalhormones101.com/
Disclaimer click here: http://www.drdach.com/wst_page20.html
The reader is advised to discuss the comments on these pages with
his/her personal physicians and to only act upon the advice of his/her
personal physician. Also note that concerning an answer which appears as
an electronically posted question, I am NOT creating a physician —
patient relationship.
Although identities will remain confidential as much as possible, as I
can not control the media, I can not take responsibility for any
breaches of confidentiality that may occur.
Link to this article
Copyright (c) 2014 Jeffrey Dach MD All Rights Reserved
This article may be reproduced on the internet without permission,
provided there is a link to this page and proper credit is given.
FAIR USE NOTICE: This site contains copyrighted material the use of
which has not always been specifically authorized by the copyright
owner. We are making such material available in our efforts to advance
understanding of issues of significance. We believe this constitutes a
‘fair use’ of any such copyrighted material as provided for in section
107 of the US Copyright Law. In accordance with Title 17 U.S.C. Section
107, the material on this site is distributed without profit to those
who have expressed a prior interest in receiving the included
information for research and educational purposes.
Serving Areas of: Hollywood, Aventura, Miami, Fort Lauderdale,
Pembroke Pines, Miramar, Davie, Coral Springs, Cooper City, Sunshine
Ranches, Hallandale, Surfside, Miami Beach, Sunny Isles, Normandy Isles,
Coral Gables, Hialeah, Golden Beach ,Kendall,sunrise, coral springs,
parkland,pompano, boca raton, palm beach, weston, dania beach, tamarac,
oakland park, boynton beach, delray,lake worth,wellington,plantation
s.
|
 PCOS Polycystic Ovary Syndrome
PCOS Polycystic Ovary Syndrome  Clinical Signs and Symptoms Of PCOS
Clinical Signs and Symptoms Of PCOS How Do You Know If You Have PCOS?
How Do You Know If You Have PCOS?  What Causes PCOS ?
What Causes PCOS ?  Oral Contraceptives
Oral Contraceptives  JeriLynn Prior MD Says: “The
fundamental problem with PCOS is not making progesterone for two weeks
every cycle. This lack of progesterone leads to an imbalance in the
ovary, causes the stimulation of higher male hormones and leads to the
irregular periods and trouble getting pregnant. Progesterone is usually
missing—replacing it therefore makes sense. “
JeriLynn Prior MD Says: “The
fundamental problem with PCOS is not making progesterone for two weeks
every cycle. This lack of progesterone leads to an imbalance in the
ovary, causes the stimulation of higher male hormones and leads to the
irregular periods and trouble getting pregnant. Progesterone is usually
missing—replacing it therefore makes sense. “  John R Lee MD says:
John R Lee MD says:  Above quote is attributed to Jerilyn Prior MD Web Site.(3)
Above quote is attributed to Jerilyn Prior MD Web Site.(3) Left Image: Polycystic ovary on ultrasound image.
Left Image: Polycystic ovary on ultrasound image.
 Useful Tools for Patients:
Useful Tools for Patients: